
Best IVF Treatment India | Female First Hospital
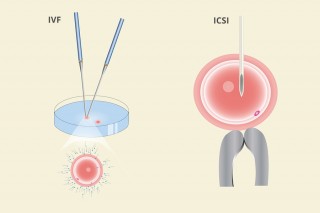
STEPS OF IVF [in vitro fertilization]
- IVF techniques can differ from clinic to clinic, Best IVF Treatment India often depending on your
individual circumstances. - A typical IVF Hospital in Surat may be involve:
For women:
Step-1: Suppressing the natural monthly hormone cycle As a first step of the IVF process you may be given a drug to suppress your natural cycle.
- Treatment is given as a Daily Injection.
- This continues for about two weeks.
Step-2: Boosting the egg supply
- After the natural cycle is suppressed you are given a fertility hormone called recombinant FSH/ highly purified FSH/ HMG (or Follicle Stimulating Hormone). This is usually taken as a daily injection for around 12 -14 days
- ALONG WITH THAT GNRH AGONIST OR ANTAGONIST HORMONE INJECTIONS ARE GIVEN.
- SOMETIMES TO IMPROVE QUALITY OF EGG IN POOR RESPONDER CASES GROWTH HORMONE INJECTIONS GIVEN.
- This hormone will increase the number of eggs you produce – meaning that more eggs can be retrieved and fertilized. With more fertilized eggs, the clinic has a greater choice of embryos to use in the treatment.
Step 3: Checking on progress
- Throughout the drug treatment, the clinic will monitor the progress. This is done by vaginal ultrasound scans and, possibly, blood tests and trigger (hormone) injection will be given for final maturation of eggs (usually more than 3 follicles of greater than 18mm in size).
Step 4: Collecting the eggs
- After 34-36 hours of trigger injection, the eggs are usually collected by ultrasound guidance under sedation and general anesthesia. This involves a needle being inserted into the scanning probe and into each ovary, The eggs are, in turn, collected through the needle.
- Cramping and a small amount of vaginal bleeding can occur after the procedure.
For Man:
Step-5; Fertilizing the eggs
- Collected eggs are mixed with husband’s sperm and cultured in the laboratory for 16–20 hours. They are then checked to see for fertilization.
- Those that have been fertilized (now called embryos) are grown in the laboratory incubator for another one – two days before being checked again. The best THREE embryos will then be chosen for transfer.
- After egg collection, medication is given to help prepare the lining of the womb for embryo transfer. This is given as pessaries, injection or gel AND TABLETS.
Step-6: Embryo transfer
- One or two or three embryos can be transferred.
- The number of embryos is restricted because of the risks associated with multiple births. Remaining embryos may be frozen for future IVF attempts, if they are suitable
Step-7: Other treatments
- Some clinics may also offer blastocyst transfer, where the fertilized eggs are left to mature for five to six days and then transferred.
ICSI [ Intracytoplasmic Sperm Injection]
Definition of ICSI
ICSI is a procedure where the embryologist directly injects a single sperm into the egg for fertilization. This may be helpful in cases where there is poor quality sperm from the male partner, or where there is an issue with the egg where fertilization can’t occur due to changes in the membranes surrounding the egg.
ICSI is an acronym for intracytoplasmic sperm injection. IVF with ICSI involves the use of specialized micromanipulation tools and equipment and inverted microscopes that enable embryologists to select and then pick up individual sperms in a tiny specially designed hollow ICSI needle. Then the needle is carefully advanced through the outer shell of the egg and egg membrane and the sperm is then injected into the inner part (cytoplasm) of the egg. This will usually result in fertilization in approximately 70-85% of eggs injected with viable sperm.
Using micromanipulation technology, ICSI allows fertility specialists to fertilize an egg using just one sperm. While it is preferred to use sperm from a semen sample, specialists can retrieve sperm from the testicles if it is necessary. This process bypasses the conventional IVF methods of fertilization, thereby ensuring that fertilization has taken place. The fertilized eggs are then left to culture for a few days before being transferred back to the woman’s uterus. ICSI is always used alongside IVF.
Indications for ICSI
- Couples who have had unexplained fertilization failure in a previous IVF cycle.
- Decreased sperm concentration, providing enough viable sperm can be recovered for injection of eggs.
- Decreased sperm motility, including totally immotile sperm (e.g. Kartagener’s syndrome), providing sperm are viable.
- Unusually high percentage of morphologically abnormal sperm, including round- headed sperm (globoazoospermia).
- Complete absence of sperm in the ejaculate due to an obstruction (obstructive azoospermia) caused by conditions such as congenital absence of the vas deferens (CAVD), post-inflammatory obstruction of the epididymis or vas and failed vasectomy reversal. Testicular sperm extraction (TESE) is used to retrieve sperm for ICSI.
- Complete absence of sperm in the ejaculate due to defective sperm production (non- obstructive azoospermia). Patients who have normal sperm formation in at least some areas of the testis (identified by testicular biopsy), providing enough viable sperm can be retrieved with TESE.
- Ejaculatory dysfunction caused by retrograde ejaculation (enough sperm are usually recovered from the urine) or paraplegia (electroejaculation or TESE).
- Immunological factors; antisperm antibodies in female sera, follicular fluid or on sperm caused by vasectomy or genital tract infection.
- Testicular cancer patients with semen samples frozen prior to treatment.
How is ICSI Performed?
- The mature egg is held with a specialized holding pipette.
- A very delicate, sharp and hollow needle is used to immobilize and pick up a single sperm.
- This needle is then carefully inserted through the zona (shell of egg) and in to the cytoplasm of the egg.
- The sperm is injected in to the cytoplasm and the needle carefully removed.
- The eggs are checked the next morning for evidence of normal fertilization.
